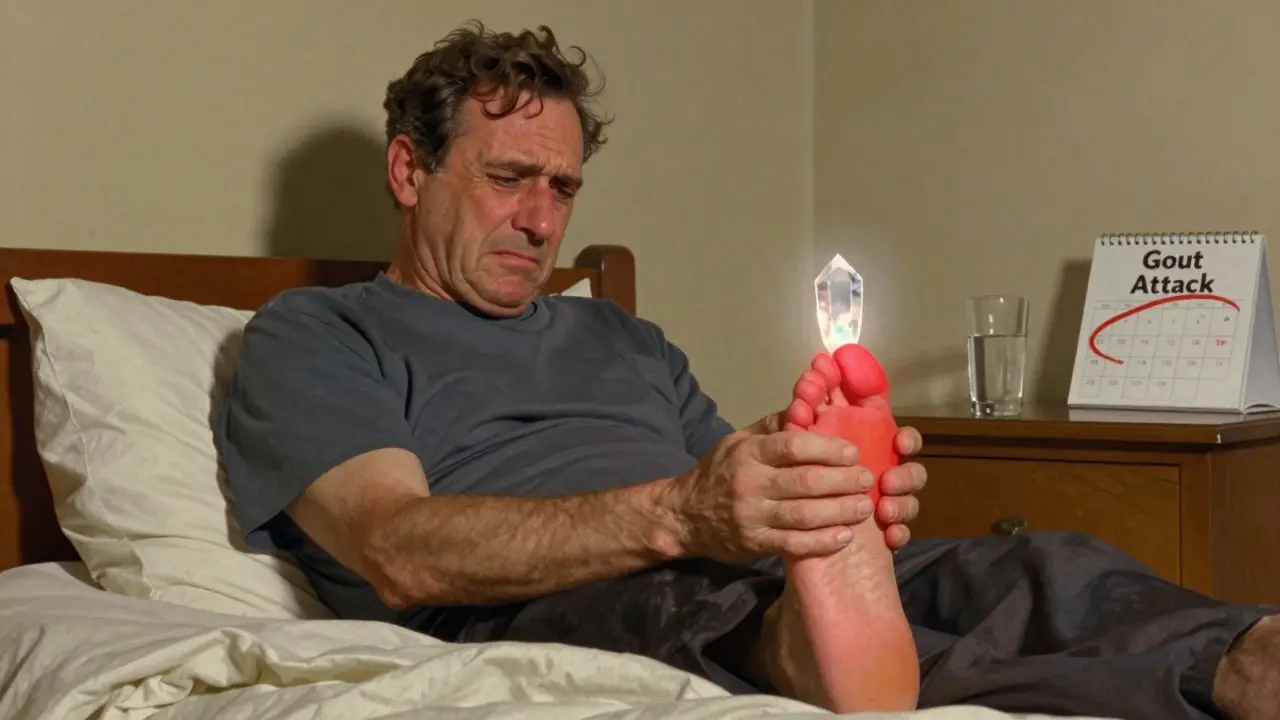
When your big toe suddenly feels like it’s on fire-swollen, red, and so tender that even a bedsheet feels unbearable-you’re likely experiencing a gout attack. This isn’t just a bad case of arthritis. It’s your body’s immune system going into overdrive because of tiny, sharp crystals forming in your joint. These crystals are made of monosodium urate (a form of uric acid that crystallizes when levels in the blood get too high), and they don’t appear out of nowhere. They build up slowly, often for years, before suddenly triggering intense pain. Understanding what causes these attacks, what makes them worse, and how to treat them properly can change your life.
Why Uric Acid Builds Up: It’s Not Just Diet
Many people think gout is caused by eating too much steak or drinking too much beer. While those things can play a role, they’re only part of the story. The real issue is how your body handles uric acid. Uric acid is a waste product made when your body breaks down purines-substances found naturally in your cells and in certain foods. Most people clear it out through their kidneys. But in about 90% of gout cases, the problem isn’t that you make too much uric acid-it’s that your kidneys don’t flush it out fast enough.
This isn’t random. Genetics play a huge part. Studies show that up to 60% of differences in uric acid levels between people come from inherited traits. Specific genes like SLC2A9 (a kidney transporter that reabsorbs uric acid) and ABCG2 (a transporter that helps dump uric acid into urine) can make your kidneys hold onto more uric acid than they should. Even if you eat perfectly, your body might still be wired to keep uric acid levels too high.
There’s also a biological threshold: 6.8 mg/dL. That’s the point at which uric acid becomes too concentrated to stay dissolved in your blood. Once you cross it, crystals start forming. And once they form, they can sit in your joints for years without causing problems-until something triggers them.
What Actually Triggers a Gout Attack?
It’s not enough to have high uric acid. Something has to shake loose those crystals. And surprisingly, it’s often a change in uric acid levels-whether they go up or down-that sets off an attack.
- Dehydration: If you’re not drinking enough water, your urine output drops below 1.5 liters a day. That means uric acid gets more concentrated in your blood and kidneys, pushing you over the saturation point. A single hot day without enough fluids can be enough.
- Starting or changing urate-lowering meds: This is one of the most misunderstood triggers. If you start taking allopurinol or febuxostat to lower uric acid, your body reacts. The crystals start dissolving, and your immune system sees them as invaders. About 30-40% of people get a flare in the first 6 months of treatment-not because the medicine isn’t working, but because it’s working too well.
- Joint injury or stress: Even a minor bump or overuse of a joint can dislodge crystals. That’s why gout often hits the big toe-it’s a joint that gets bumped often.
- Alcohol: Beer is the worst offender. Each 12-ounce serving increases your risk by 49%. That’s because beer contains not just alcohol, but also high levels of purines from yeast. Spirits are less risky (15% increase per serving), and wine has little to no effect.
- Fructose: Sugary drinks-soda, energy drinks, sweetened juices-trigger uric acid production by breaking down ATP in your liver. Just one sugary drink a day can raise your risk by 20-30%.
- Purine-rich foods: Organ meats like liver and kidney have 300-500 mg of purines per 3-ounce serving. Shellfish like shrimp and mussels are also high. Red meat contributes too, but not as dramatically as beer or sugary drinks.
What’s surprising? Dairy doesn’t trigger gout-it helps. One daily serving of low-fat milk or yogurt cuts your risk by 43%. The exact reason isn’t fully known, but it’s likely related to proteins in milk that help the kidneys excrete uric acid.
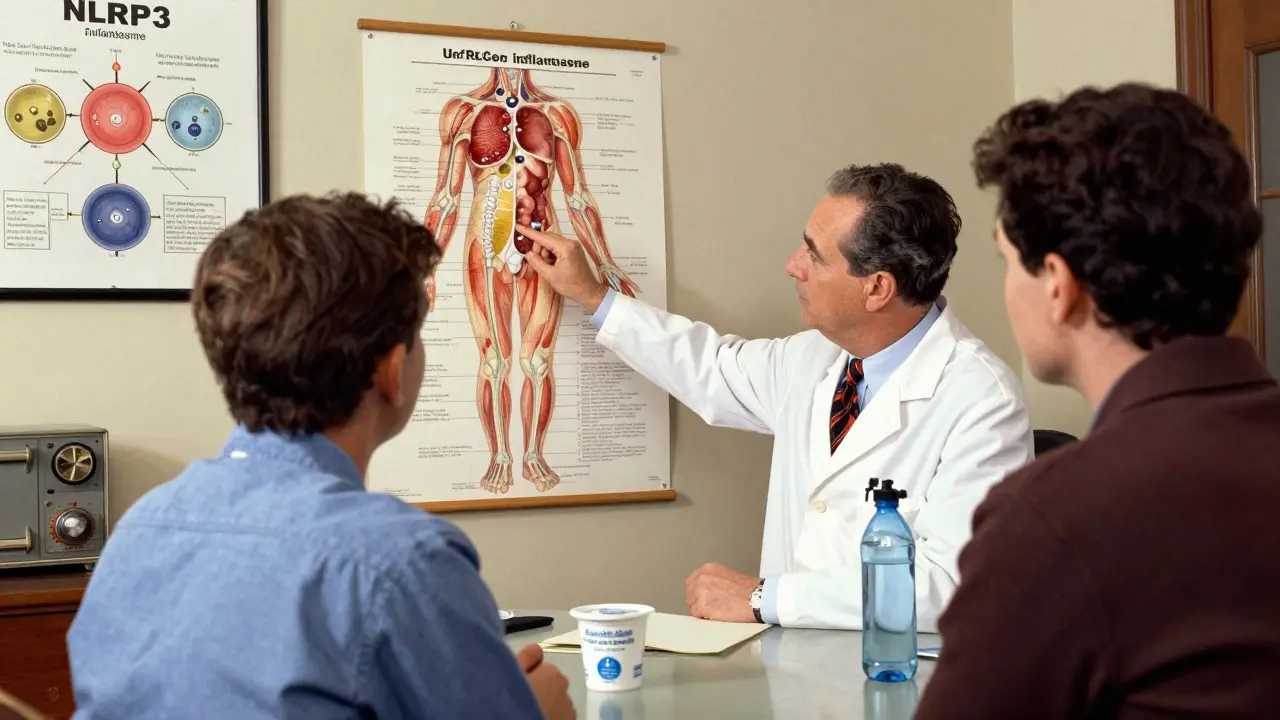
How Gout Attacks Actually Happen: The Inflammation Cascade
When a crystal breaks loose, your immune system doesn’t just notice-it goes nuclear. Special immune cells called macrophages recognize the crystals and activate something called the NLRP3 inflammasome (a protein complex that triggers inflammation). This turns on a chain reaction that releases interleukin-1β, a powerful inflammatory signal. That’s what causes the swelling, heat, and excruciating pain.
That’s why anti-inflammatory drugs work so well. NSAIDs like indomethacin, colchicine, and corticosteroids don’t lower uric acid-they stop the immune response. That’s why you can’t just pop a pill and expect the pain to vanish instantly. It takes time for the inflammation to calm down.
Medication Strategies: Acute Attacks vs. Long-Term Control
Treating gout has two phases: stopping the attack and preventing the next one. They require completely different approaches.
During an Attack: Stop the Fire
There are three main options for treating an acute flare:
- NSAIDs: Indomethacin (50 mg three times a day) is common. Naproxen works too. These reduce pain and swelling fast but can irritate your stomach or kidneys if you’re not careful.
- Colchicine: Taken at 0.6 mg three times a day for a few days. It blocks the immune response triggered by crystals. Side effects? Diarrhea. Up to 20% of people can’t tolerate it at full dose. Lower doses (0.6 mg once or twice daily) are often just as effective with fewer side effects.
- Corticosteroids: If you can’t take NSAIDs or colchicine, oral prednisone (30-40 mg daily for 5 days) or a joint injection works well. This is especially helpful for people with kidney disease or stomach ulcers.
Important: Don’t start or stop urate-lowering drugs during an attack. That’s a common mistake. If you’re on allopurinol and get a flare, keep taking it. Stopping it won’t help-and might make things worse later.
Long-Term: Lower the Uric Acid
Once the pain is gone, the real work begins: lowering your uric acid to prevent future attacks and dissolve existing crystals.
- Allopurinol: This is the first-line drug. Start at 100 mg daily. Increase by 100 mg every 3-4 weeks until your uric acid is below 6 mg/dL. Most people need 300-600 mg daily. Some need up to 800 mg. It’s safe for most people, even those with kidney disease.
- Febuxostat: Used if you can’t tolerate allopurinol. Dose is 40-80 mg daily. It’s more expensive and carries a slightly higher risk of heart problems, so it’s not first-choice for everyone.
- Probenecid: This helps your kidneys flush out more uric acid. Only works if your kidneys are still working well (GFR above 50 mL/min). Not for people with kidney stones.
Target? Below 6 mg/dL. For people with tophi (visible lumps of crystals under the skin), aim for 5 mg/dL or lower. Studies show that keeping uric acid below 5 mg/dL for a year leads to complete disappearance of tophi in 70% of cases.
The Most Important Rule: Prophylaxis During Treatment
If you’re starting allopurinol or febuxostat, you must take a preventive anti-inflammatory drug for at least 6 months. This isn’t optional. Without it, you’re likely to have flares.
Low-dose colchicine (0.6 mg once or twice daily) is the standard. It reduces flare frequency by 50-75% compared to no treatment. Studies like the 2007 CONFIRMS trial proved this. Many doctors skip this step-often because they don’t realize how common flares are at the start of treatment. Don’t be one of them.
What About Diet and Lifestyle?
Diet alone won’t cure gout, but it can make a big difference.
- Drink at least 2 liters of water daily. This helps your kidneys flush out uric acid.
- Limit beer to less than one 12-ounce serving per day. Avoid it entirely if you’ve had multiple attacks.
- Avoid sugary drinks. Choose water, tea, or coffee instead.
- Eat more low-fat dairy. One serving a day cuts your risk significantly.
- Reduce red meat and shellfish. You don’t have to eliminate them, but don’t make them a daily habit.
- Don’t fast or follow extreme low-calorie diets. Rapid weight loss can spike uric acid.

Why Adherence Matters More Than You Think
Here’s the hard truth: if you stop taking your urate-lowering medication, your uric acid will climb back to its old level in just 2-4 weeks. That means another attack is coming. Many people stop because they feel fine. But gout doesn’t go away-it just hides. The crystals are still there. And they’re waiting.
Also, don’t confuse symptom relief with cure. If your toe stops hurting after a flare, that doesn’t mean you’re healed. It means the inflammation calmed down. The underlying problem-high uric acid-is still there. Only consistent, long-term treatment can prevent joint damage, tophi formation, and kidney problems.
What’s Next? Emerging Treatments
Researchers are now targeting the inflammation pathway itself. New drugs like dapansutrile, which directly blocks the NLRP3 inflammasome, have shown promise in clinical trials, cutting flare duration by 40% compared to placebo. These won’t replace allopurinol, but they could become powerful tools for people who don’t respond well to current treatments.
Another exciting area is the gut microbiome. Early studies suggest certain probiotics may help break down purines in the intestines, lowering uric acid by 10-15%. This isn’t a treatment yet-but it’s a sign that future options may go beyond just the kidneys and liver.
Final Takeaway: Gout Is Manageable, But Not Curable
You can’t reverse the genetic factors that make you prone to gout. But you can control the outcome. With the right medication, consistent lifestyle changes, and strict adherence to your treatment plan, you can live without flares. The key is understanding that gout isn’t an event-it’s a chronic condition that requires daily management. The pain you feel today? It’s a warning. The crystals dissolving over time? That’s your victory. Stay the course, and your joints will thank you.
Can gout be cured with diet alone?
No. While diet can reduce flare frequency, it’s rarely enough to lower uric acid below the 6 mg/dL threshold needed to prevent attacks. Most people need medication to get their levels low enough, especially if they’ve had multiple attacks or have tophi. Diet works best as a supplement to medication, not a replacement.
Why do gout flares happen when I start taking allopurinol?
When allopurinol lowers your uric acid, crystals in your joints begin to dissolve. Your immune system sees these loosened crystals as foreign invaders and triggers inflammation. This causes a flare. That’s why doctors recommend taking low-dose colchicine for the first 6 months of treatment-it prevents these flares without stopping the medication.
Is it safe to take NSAIDs long-term for gout?
NSAIDs are meant for short-term use during flares, not daily prevention. Long-term use can damage your kidneys, raise blood pressure, or cause stomach ulcers. For long-term control, you need urate-lowering drugs like allopurinol, not daily NSAIDs.
How often should I get my uric acid tested?
When starting or adjusting medication, test every 2-5 weeks until your level is below 6 mg/dL. Once stable, check every 6 months. If you miss a dose or change your diet significantly, test sooner. Your target is lifelong control-not just a number on one test.
Can gout damage my kidneys?
Yes. Chronic high uric acid can lead to kidney stones and, over time, kidney damage. Uric acid crystals can form in the kidneys themselves, and the inflammation from repeated gout attacks can harm kidney tissue. That’s why controlling uric acid isn’t just about your joints-it’s about protecting your whole body.
If you’ve had more than two gout attacks in a year, or if you have visible tophi or joint damage on imaging, you should be on long-term urate-lowering therapy. Don’t wait until it gets worse. Talk to your doctor about your uric acid level, your medication plan, and how to stay on track. Gout doesn’t have to control your life.





Stephen Rudd
7 March 2026This post is textbook medical propaganda. Uric acid isn't the enemy - the pharmaceutical industry is. They sell you allopurinol because it's profitable, not because it works. I've been off meds for 7 years and only drink water, eat greens, and avoid sugar. My gout? Gone. No flares. No pills. No doctor visits. You're being manipulated into lifelong dependency. The system doesn't want you cured - it wants you dosed.
Erica Santos
8 March 2026Oh wow. So the real villain isn't the beer or the shrimp - it's your kidneys' inability to do their job? How revolutionary. Next you'll tell me the sun rises in the east because physics, not because the earth is flat. I'm shocked. Shocked, I tell you.
George Vou
9 March 2026i heard from this guy on youtube that gout is caused by 5g of aspartame in your soda. also the government put fluoride in the water to make your kidneys weak so they can sell you pills. my uncle had gout and he just stopped eating meat and now he's fine. also i think the doctor is lying. why do they always want you to take more pills?
Scott Easterling
9 March 2026Let's be real. The whole 'uric acid = bad' narrative is a scam. You think your kidneys are just lazy? Nah. They're being poisoned by processed food, glyphosate, and corporate toxins. Allopurinol? That's just a Band-Aid on a bullet wound. And colchicine? It's like putting duct tape on a ruptured pipe. The real fix? Detox. Fasting. Raw foods. But nope - the system wants you hooked. They don't want you healthy. They want you compliant.
Mantooth Lehto
11 March 2026I had my first gout attack last year and I was in tears. I thought I was dying. I didn't know it was from my soda habit. I stopped drinking it. I started drinking water. I cried again - but this time from relief. I still take my colchicine. I still go to my doctor. I'm not brave. I'm just smart. And I'm not alone. You're not weak for needing help. You're human.
Melba Miller
11 March 2026I live in America. We don't get to choose our healthcare. We get to choose which pill we can afford. My insulin costs more than my rent. My gout meds? I skip doses. I don't have a choice. So don't lecture me about 'adherence.' You don't know what it's like to pick between food and your life. This isn't a lifestyle. It's a survival game. And the rules? Written by people who don't live here.
Katy Shamitz
12 March 2026I just want to say - if you're reading this and you're struggling with gout, you're not alone. I've been there. I used to think it was my fault. I thought I was lazy. I thought I was weak. But it's not about willpower. It's about biology. And healing isn't about punishment - it's about patience. One day at a time. One sip of water. One pill. One step. You're doing better than you think.
Nicholas Gama
13 March 2026The 6.8 mg/dL threshold is a statistical artifact. Not a biological law. The entire field of rheumatology is built on flawed assumptions. You think crystals form at 6.8? That's a population mean. Not a universal trigger. Individual saturation points vary. But we don't test individuals. We test populations. And then we medicate. This isn't medicine. It's mass compliance.
Mary Beth Brook
14 March 2026NLRP3 inflammasome activation is the central pathophysiological driver. IL-1β is the key cytokine. The therapeutic rationale for colchicine is microtubule disruption, which inhibits neutrophil chemotaxis and pyroptosis. Allopurinol's xanthine oxidase inhibition reduces purine catabolism. Probenecid enhances renal excretion via URAT1 inhibition. These are evidence-based interventions. Not opinions. Not anecdotes. Science.
Neeti Rustagi
15 March 2026I am from India, and in our traditional Ayurvedic practice, we have long understood that gout is linked to ama, or toxins, formed from poor digestion. We use ginger, turmeric, and guggul to support liver and kidney function. Medication is helpful, yes - but lifestyle is foundational. A balanced diet, proper hydration, and mindful living are not optional. They are the pillars of health. May you find peace in both science and tradition.
Dan Mayer
16 March 2026i think the real problem is that doctors dont tell you that allopurinol can cause a rash that kills you. i had a friend who got it and he died. no one warned him. now im scared to take anything. also i heard gout is caused by wifi. is that true?
Ray Foret Jr.
17 March 2026I was skeptical at first, but this post changed my whole outlook. I started on allopurinol last month and took the colchicine like they said. No flares. Not one. I didn't think it would work. I thought I'd have to suffer forever. Turns out, I just needed to trust the process. You're not broken. You're just healing. Keep going. You got this. 🙌
Samantha Fierro
19 March 2026I appreciate how thoroughly this was explained. As a nurse who works with chronic disease patients, I see daily how misunderstood gout is. Many believe it's 'just a bad toe' - when in reality, it's a systemic inflammatory condition with far-reaching implications. The emphasis on adherence, prophylaxis, and long-term uric acid control is not just correct - it's lifesaving. Thank you for this clear, compassionate guide. You've made a difference today.
Robert Bliss
21 March 2026I used to think gout was just from drinking too much beer. Then I got it. And I realized - it's not about what you eat. It's about what your body can't get rid of. I changed my life. Water. No soda. Low-fat milk. And yes, I take my meds. I'm not perfect. But I'm trying. And that's enough.
Peter Kovac
22 March 2026The data is clear: 90% of gout cases stem from renal underexcretion. Genetic polymorphisms in SLC2A9 and ABCG2 account for 60% of population variance in serum urate. Urate-lowering therapy reduces tophi regression time by 70% when maintained below 5 mg/dL. NSAIDs are first-line for acute flares, but lack disease-modifying properties. Colchicine prophylaxis reduces flare incidence by 50–75%. These are not opinions. They are meta-analyzed, peer-reviewed, clinically validated facts. Stop treating gout like a lifestyle choice. It is a metabolic disorder. Treat it like one.